 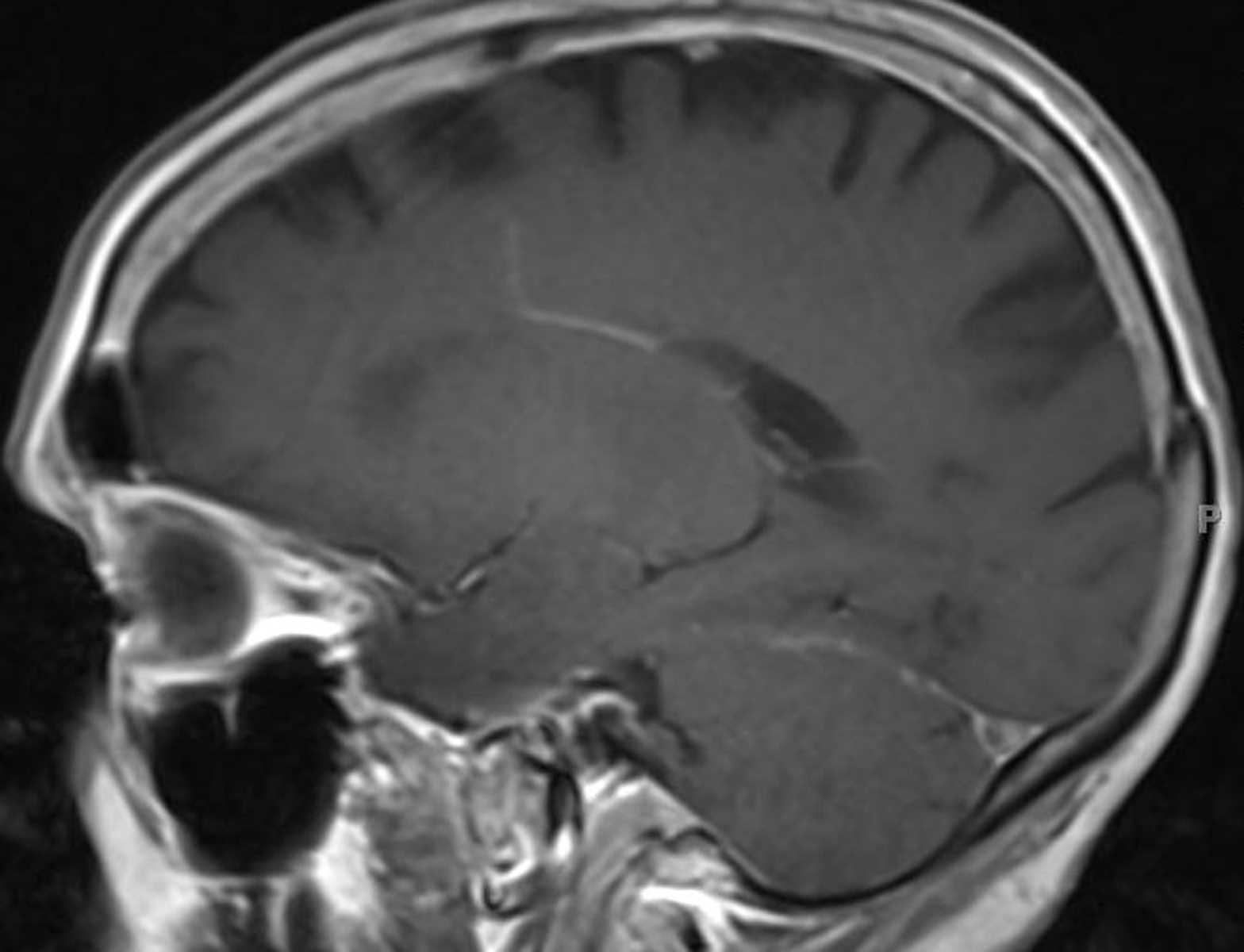
CCMs are angiographically occult lesion, and cerebral digital subtraction angiography is the gold standard for the diagnosis of DVA. Mixed CCM with DVA has a higher risk of hemorrhage. DVAs are benign lesions by nature however, venous infarction can occur in a few patients due to acute thrombosis. CCM can have a wide array of clinical presentations like hemorrhage, seizures, or focal neurological deficits or can also be an incidental finding on brain imaging. Summary: The search yielded 1,249 results for “Cerebral cavernous malformations,” 271 results for “Developmental venous anomaly,” and 5 results for “Mixed Cerebral cavernous malformations with Developmental venous anomaly.” DVA is the most common intracranial vascular malformation, followed by CCM. All studies in the English language in the past 10 years were analyzed descriptively for this review. A PubMed search using the keywords “Cerebral cavernous malformations, Developmental venous anomaly, Mixed Cerebral cavernous malformations with Developmental venous anomaly” was done. In this paper, we aim to give a comprehensive review of CCM, DVA, and their coexistence as mixed lesions. The most common mixed form is the coexistence of CCM with an associated developmental venous anomaly (DVA). Background: Cerebral cavernous malformations (CCMs) are intracranial vascular malformations that can exist as a single lesion or mixed vascular lesions. Although there is no pathognomonic nystagmus associated with DVAs, nystagmus of many forms can be shown including single-sided gaze nystagmus, GEN, and upbeating nystagmus at particular gaze. Hypometric saccade movement in both directions seems compatible with a dysfunction of the affected area. The location of DVAs was also adjacent to paramedian pontine reticular formation along with the vestibular nuclei complex which organizes the neuronal information in saccade pathway. Venous hypertension can be transient and repetitive provoking recurrent attacks. Venous congestion and interstitial edema around the lesion can cause imbalance of vestibular firing rate of the vestibular nuclei complex, which can result in vertigo attack. The DVAs of the patient was located adjacent to the vestibular nuclei complex. The vestibular nuclei complex is mainly located in the pons extending rostrally to the floor of the cerebellum and caudally into the medulla. Our patient presented with spontaneous recurrent vertigo accompanied by moderate headache of both temporal areas. Conservative management for symptom control with regular follow-up appointments was recommended. The patient reported partial resolution of symptoms with medication in less than 50% of vertigo attacks. Empirical treatment to alleviate symptoms with beta- adrenergic blocking agents to lower the blood pressure in enlarged veins in DVAs was followed. The DVAs were considered to be the cause of clinical symptoms because all other causes were excluded at physical examination, the audio-vestibular function test, and the radiologic examination. Axial T1-weighted turbo spin-echo gadolinium MRI showed a vascular-like enhancement presenting radicular divisions in the pons extending to medulla oblongata having a caput medusae appearance ( Fig. There was no evidence of a cavernous angioma, hemorrhage, acute parenchymal injury, or edematous changes. The MRI with angiography revealed DVAs in the right ventral pons and medulla in proximity to the vestibular nuclei complex. In addition, caloric test showed mild right-sided weakness with canal paresis ratio of 22.09%, but vHIT showed normal findings at three semicircular canals ( Fig. In the saccadic eye movement test, hypometria was predominantly observed on the right eyeball in bilateral horizontal measurements ( Fig. Video nystagmography showed neither spontaneous nystagmus nor gaze-evoked nystagmus (GEN). Pure tone audiometry showed normal hearing status. During the evaluation, pure tone audiometry, vestibular function test including video nystagmography, caloric test, video head impulse test (vHIT), and magnetic resonance imaging (MRI) with angiography were performed. The physical examination and otoscopy yielded normal findings. She had no current or previous history of migraine and the clinical symptoms did not fulfill the criteria of vestibular migraine according to the Barany Society and the International Headache Society. A 15-year-old girl presented with a 5-year history of recurrent vertigo that occurred more than three times a day and lasted about 15 minutes, accompanied by moderate headache of both temporal areas.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
